|
3/30/2023 0 Comments Stapled anastomosis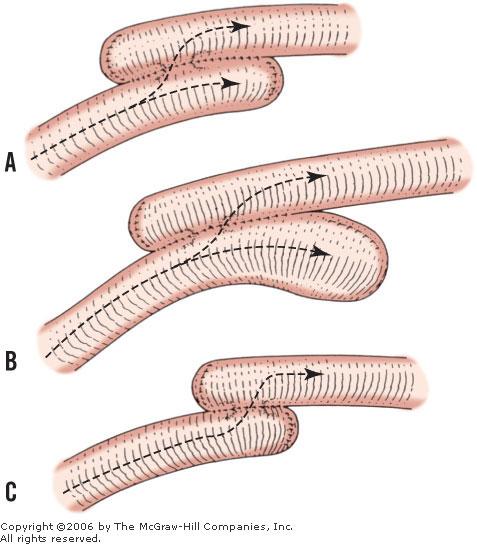
The specimens were removed through left lower quadrant incision. All procedures were carried out without conversion to conventional laparotomy. Q.) and were completed laparoscopically with his surgical group. All operations were performed by a single surgeon (S. The patients included were staged for stage II or III according to the UICC/AJCC classification (8th Edition) and underwent an anterior resection of the proximal rectum and the distal sigmoid colon with a sigmoidorectostomy. The collective consisted of 83 females and 121 males. The resulting 204 patients had a mean age of 63.2 ± 11.6 years and a mean BMI of 22.8 ± 2.1. Among these 247 patients, 43 cases were excluded for meeting the exclusion criteria. In total, 247 patients underwent resection for colorectal cancer followed by circular stapler anastomosis in Tongren Municipal People’s Hospital of Guizhou Medical University during the period from 10 August 2020 to 12 August 2021. The minimal height of the anastomotic rings as indicator for technically insufficient anastomoses is a good predictor of AL, while postoperatively the NLR was superior to the CRP in prediction of AL. Still, it was superior to the NLR at POD 3 (0.74) and the CRP at POD 3 (ROC-AUC 0.54) and 5 (ROC-AUC 0.70). The minimal height of the anastomotic rings as a binary classifier had a good ROC-AUC of 0.81 but was inferior to the NLR at postoperative day (POD) 5, with an excellent ROC-AUC of 0.93. We included 204 patients, of which 19 suffered from anastomotic leakage (LEAK group), while in 185 patients the anastomoses healed well (HEAL group). The predictive value of the anastomotic ring configuration and the neutrophil-to-lymphocyte ratio (NLR) regarding anastomotic leakage is examined by ROC analyses and compared to the C-reactive protein (CRP) as an established marker. We perform a prospective single-center cohort study, including patients undergoing stapled circular anastomosis between August 2020 and August 2021. Here, we aim to quantitatively investigate the morphology of anastomotic rings as an early available prognostic marker for AL and compare them to established inflammatory markers. 
Cochrane Central Register of Controlled Trials (CENTRAL).Reliable markers to predict or diagnose anastomotic leakage (AL) of stapled circular anastomoses following colorectal resections are an important clinical need. (2017)Prospective Randomized Study of the Kono‐S Anastomosis Versus the Side‐to‐side Functional End Anastomosis in the Prevention of Post‐operative Recurrence of Crohn's Disease. Ravitch MM, Steichen FM (1972) Technics of staple suturing in the gastrointestinal tract. Simillis C, Purkayastha S, Yamamoto T, Strong SA, Darzi AW, Tekkis PP (2007) A meta-analysis comparing conventional end-to-end anastomosis vs other anastomotic configurations after resection in Crohn’s disease. Ng CH, Chin YH, Lin SY, Koh JWH, Lieske B, Koh FH et al (2021) Kono-S anastomosis for crohn’s disease: a systemic review, meta-analysis, and meta-regression. Luglio G, Rispo A, Imperatore N, Giglio MC, Amendola A, Tropeano FP et al (2020) Surgical prevention of anastomotic recurrence by excluding mesentery in crohn’s disease: the SuPREMe-CD study - a randomized clinical trial. Yamamoto T (2013) A new anastomotic technique for prevention of postoperative recurrence in Crohn’s disease. Gut 25(6):665–672įichera A, Zoccali M, Kono T (2012) Antimesenteric functional end-to-end handsewn (Kono-S) anastomosis. Rutgeerts P, Geboes K, Vantrappen G, Kerremans R, Coenegrachts JL, Coremans G (1984) Natural history of recurrent Crohn’s disease at the ileocolonic anastomosis after curative surgery. McLeod RS, Wolff BG, Ross S, Parkes R, McKenzie M, Investigators of the CT (2009) Recurrence of Crohn’s disease after ileocolic resection is not affected by anastomotic type: results of a multicenter, randomized, controlled trial. Rutgeerts P, Goboes K, Peeters M, Hiele M, Penninckx F, Aerts R et al (1991) Effect of faecal stream diversion on recurrence of Crohn’s disease in the neoterminal ileum. Wolford DD, Fichera A (2020) Prophylaxis of Crohn’s disease recurrence: a surgeon’s perspective. Kalman TD, Everhov AH, Nordenvall C, Sachs MC, Halfvarson J, Ekbom A et al (2020) Decrease in primary but not in secondary abdominal surgery for Crohn’s disease: nationwide cohort study, 1990–2014. Yao JY, Jiang Y, Ke J, Lu Y, Hu J, Zhi M (2020) Development of a prognostic model for one-year surgery risk in Crohn’s disease patients: a retrospective study.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
